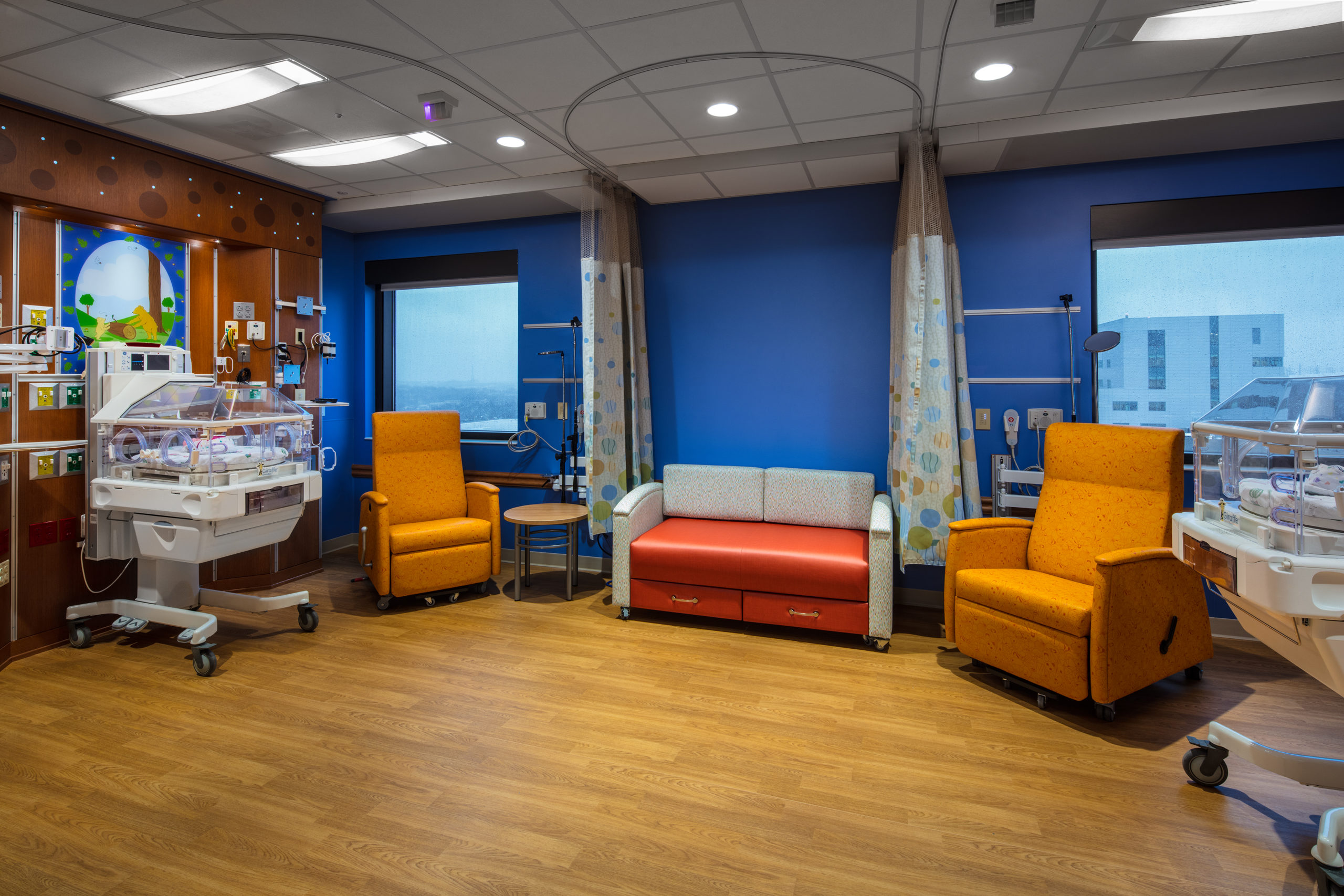
Pediatric patients have very specific needs when it comes to their healthcare treatment. As our healthcare clients often say, pediatric patients are not just small adults. They have very different physical needs, such as not having fully developed immune systems. Their families have different needs as well since a child needs their parents and family members present during treatment.
At Zimmerman, our healthcare team has many years of experience in designing pediatric healthcare spaces. Through our projects, we have experienced first-hand the importance of designing appropriate amounts of space to support pediatric patients and their families.
Support space is inversely related to patient size
It may seem counterintuitive, but the amount of space needed for family support in a pediatric inpatient room is greater than in an adult inpatient room. When an adult receives medical treatment, they usually bring one additional support person. On the other hand, children tend to have two or more family members. In addition to needing to fit everyone in the exam room, it’s important to provide adequate space in the pediatric patient rooms for families to stay overnight. Amenities such as a good sleeper sofa, storage for personal items and clothing, and a refrigerator can make the family’s stay much more comfortable.
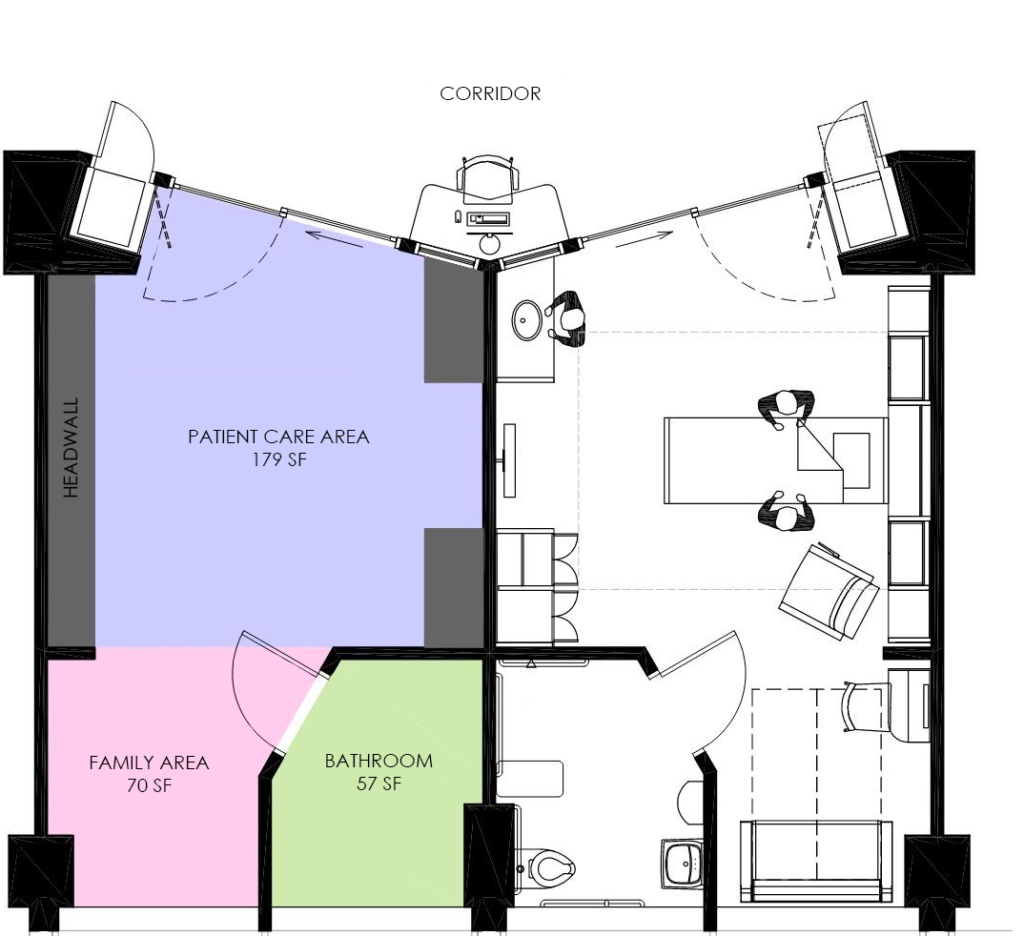
Leaning on clinical staff for support
Before visitor restrictions were implemented during COVID, the patient’s siblings would often accompany a parent for an appointment or treatment. With these new restrictions, the number of support persons for a pediatric patient is typically restricted to two adult visitors, with some facilities only allowing one visitor.
Without a larger family support network present, the parent or guardian staying with the child receiving inpatient care can need more time and attention from staff. The parent doesn’t have another family member available to care for the child while they rest or take a break, and doesn’t have another adult around to socialize with or lean on for emotional support. That family member may rely on the clinical staff for these needs, increasing staff responsibilities.
A research article published in a scientific journal found that “coping strategies used by parents include ‘acquiring social support’ and ‘mobilizing the family to acquire and accept help.’” Parent-to-parent support is a useful mechanism for enhancing well-being and deserves to be implemented in pediatric healthcare settings.
Designing spaces for psychosocial support
With the shift to private patient rooms in hospitals to help decrease the spread of COVID, we have seen improvements in increased privacy, reduced noise levels and infection presentation. However, one drawback of private inpatient rooms is that a patient’s family members are more isolated from other patient families. Families lose opportunities to connect with other families in similar situations and share their challenges.
Because of this privacy transition, we need to provide space for multiple family members and visitors in the pediatric patient room to create a psychosocial support system. Spaces outside the patient room where families can connect are also important for their well-being and emotional support.
One strategy to provide more social connection between families is to design patient rooms in ‘neighborhoods” or “pods.” Families of patients located within a “neighborhood” will have more chance encounters that can encourage interaction and socialization.
Providing support spaces such as a family lounge, kitchen, or laundry facilities on the patient unit can provide a chance for a caregiver to take a break and connect with other caregivers as well.
Relieving emotional stress through psychosocially supportive environments
The need for psychosocial support is why we need to provide space for multiple family members in the pediatric patient room so they can support each other. When family members can support each other, they don’t require as much support from clinical staff for emotional or social needs, enabling staff to focus more on direct patient care. Providing spaces for social connection outside the patient room is also important for family support. By focusing on the needs of the family as well as the patient, we can create healthcare environments that provide psychosocial support while also continuing to hold space for families in patient rooms.